The Lymphatic System and Sinus Disease
When patients ask me why their sinus infections keep coming back — why the antibiotics work for a while and then stop working, why they feel congested even when they do not have an active infection, why their face feels heavy and their head feels full even on a good day — most of them expect me to talk about bacteria, or anatomy, or allergies.
I talk about fluid.
Specifically, I talk about the lymphatic system — and why this extraordinary network of channels, nodes, and immune tissue is almost never part of the conversation when a provider is managing chronic sinus disease.
Clinical rhinology education written in plain language. Subscribe to the Airway & Sinus Wellness Review.
What the Lymphatic System Is Actually Doing
The lymphatic system is the body’s internal drainage and immune surveillance network. It moves fluid — lymph — through a series of channels and nodes that filter out pathogens, cellular debris, and inflammatory proteins, and then return the cleaned fluid back to circulation. In the head and neck specifically, the lymphatic system is doing something even more critical: it is the primary mechanism by which the mucosal surfaces of the upper airway clear the infectious and inflammatory burden that those surfaces encounter constantly.
Think about what the nasal and sinus mucosa are exposed to every day. Every breath carries allergens, particulates, bacteria, viruses, and environmental irritants across a mucosal surface that stretches from the tip of the nose to the back of the throat. The adenoids, the tonsils, the lateral pharyngeal bands, the lymphatic tissue studded throughout the airway lining — all of these structures are actively sampling what passes through and coordinating an immune response to what they find. The lymphatic channels draining these structures carry the filtered output of that immune response down through the cervical lymph node chains and ultimately into the thoracic duct and systemic circulation.
When this system is working well, you never think about it. Pathogens are captured, flagged, and eliminated before they can establish an infection. Inflammatory proteins are cleared before they accumulate enough to cause symptoms. The mucosal surfaces stay clean and functional. The sinuses drain.
When this system is not working well — when lymph flow is sluggish, when the nodes are overwhelmed, when the mucosal immune tissue is carrying a burden it cannot clear — the consequences show up in your sinuses before almost anywhere else.
Why Medicine Ignores It
In thirty-plus years of practicing otolaryngology, I have never heard a primary care physician or urgent care provider mention the lymphatic system in the context of a sinus infection. Not once. And I understand why — it is not that the lymphatic system is unimportant. It is that prescribing an antibiotic takes thirty seconds and explaining lymphatic drainage takes thirty minutes.
The antibiotic is the path of least resistance. It addresses the symptom — bacterial load — quickly and gives both the provider and the patient the feeling that something decisive has been done. The lymphatic system, which has no simple pharmaceutical target and requires patient behavior change to optimize, never comes up.
This is a significant gap in how we treat chronic sinus disease. Because the lymphatic system is not just a passive bystander in your recurring sinus infections. It is often a primary driver of why you cannot clear them.
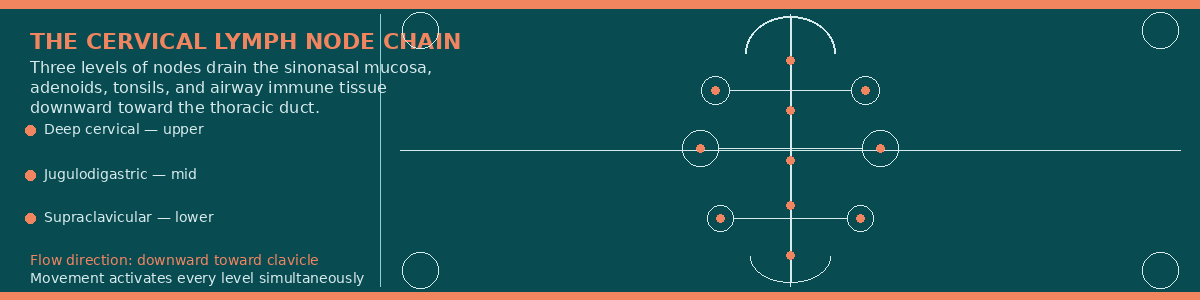
The diagram below maps the three levels of the cervical lymph node chain that drain the sinonasal mucosa, adenoids, tonsils, and airway immune tissue — showing how each level connects to the central lymphatic trunk and why flow direction matters for every drainage technique in the protocol that follows.
What I See When I Examine a Patient with Chronic Sinusitis
When I examine a patient with chronic or recurring sinusitis, I am not only looking inside the nose. I am also palpating the neck — feeling the cervical lymph node chains along both sides of the neck, from the angle of the jaw down to the clavicle.
In a healthy patient without active sinus disease, those lymph nodes are small, soft, non-tender, and barely palpable. In a patient with chronic sinusitis — particularly one who has been through multiple antibiotic courses — what I often find is different. The nodes may be enlarged. They may be tender to palpation. The soft tissue of the neck may feel thicker, less mobile, less well-defined than it should.
The first question every physician is trained to ask when they find an enlarged lymph node is: could this be cancer? And once that concern has been appropriately evaluated and excluded, the second question is: what is causing the inflammation that is making these nodes work so hard?
In my chronic sinusitis patients, the answer is almost always the same. The nodes are enlarged because they are downstream of a mucosal surface that has been inflamed for months or years. They are doing their job. The problem is that the volume of inflammatory burden they are being asked to process has exceeded their capacity to clear it efficiently — and the result is a system that is congested, sluggish, and unable to restore the patient to baseline between episodes.
What Lymphatic Congestion Actually Feels Like
When the lymphatic system in the head and neck is congested, the symptoms it produces are not always what patients expect. They often do not feel like infection. They feel like something more diffuse and harder to name.
Facial pressure and heaviness — the feeling that your face is full and your sinuses are pushing outward — is one of the most consistent symptoms. This is not always caused by mucus accumulation or bacterial infection. It is often caused by interstitial fluid and inflammatory proteins that the lymphatic system has not been able to clear from the mucosal tissue. The tissue itself is waterlogged with inflammatory byproducts that have nowhere to go.
Post-nasal drainage that does not resolve with antibiotics is another signal. When the mucosal immune tissue is overwhelmed, it continues producing secretions as part of the immune response long after the acute infectious trigger has been eliminated. The drainage is not infection — it is the immune system still working through a backlog it cannot clear efficiently.
Fatigue, brain fog, and the feeling of not being fully present are symptoms that patients often attribute to poor sleep or stress. But in a significant proportion of chronic sinus patients, these symptoms have a direct lymphatic contribution. When the cervical lymphatic system is congested, the drainage of inflammatory proteins from the brain — through the glymphatic system and ultimately into the cervical lymph nodes — is impaired. The brain is not clearing its own inflammatory waste as efficiently as it should. The cognitive and energy consequences of that impairment are real, measurable, and often significantly underestimated.
A sedentary lifestyle makes all of this dramatically worse. The lymphatic system has no pump. It depends entirely on muscle contraction, movement, and breathing to move lymph through its channels. A patient who sits for eight to ten hours a day and then sleeps for eight hours is giving their lymphatic system almost no opportunity to move the fluid that has accumulated during those hours of inactivity. In the head and neck specifically — where gravity is working against upward drainage — the effect of prolonged inactivity on lymph stagnation is significant.
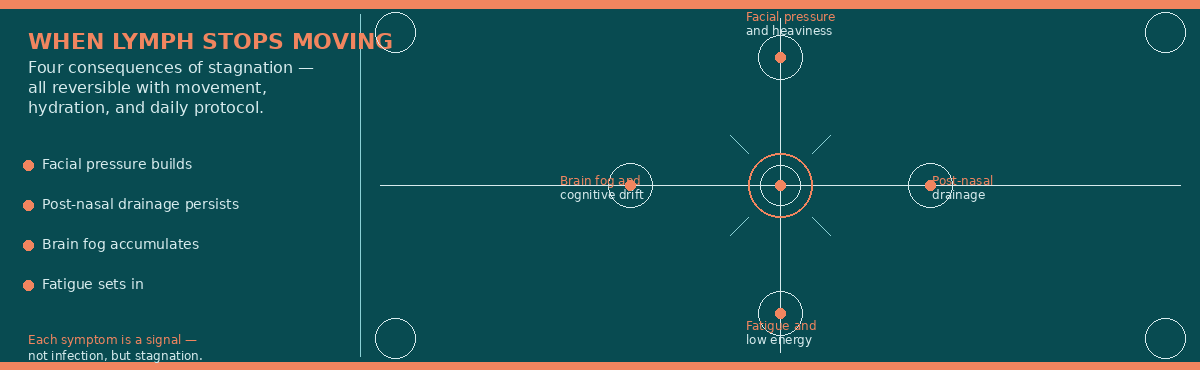
The diagram below maps the four primary consequences of lymphatic stagnation in the head and neck — each one a symptom that patients attribute to infection or stress, but that traces directly back to fluid that has stopped moving. Read across the four nodes and you will see why the same patient has facial pressure, drainage that won’t clear, brain fog, and fatigue all at once — they share a single root cause.
The Protocol — Getting the System Moving Again
The good news is that the lymphatic system responds to relatively simple interventions. Unlike the bacterial biofilm problem — which requires specific chemical disruption — the lymphatic congestion problem responds to movement, hydration, heat, and manual drainage. You can start today. You do not need a prescription.
The SAWC Daily Lymphatic Mobilization Protocol
Step 1: Move — The Toe Bounce
Exercise is the single most important thing you can do for your lymphatic system. The lymphatic system has no heart to pump it — it is entirely dependent on muscle contraction to move fluid through its channels. Any movement helps, but the simplest and most accessible daily practice is the toe bounce.
-
Stand with feet hip-width apart at the bathroom sink — morning and evening while brushing your teeth and rinsing your nose
-
Rise onto the balls of your feet and drop rhythmically — approximately one bounce per second
-
The impact travels upward through the legs, pelvis, torso, and neck — activating every muscle group as a gentle lymphatic pump
-
Two minutes is enough to meaningfully stimulate cervical lymphatic flow
-
This is the most efficient whole-body lymphatic mobilization available without equipment — and you are already standing at the sink
Step 2: Head and Neck Self-Massage — 3 Minutes
Manual drainage of the cervical lymphatic chain accelerates clearance of the inflammatory fluid that has accumulated in the facial and sinus tissue. The technique follows the anatomy of the lymphatic drainage pathway — always moving fluid toward the clavicle, never upward against the natural drainage direction.
-
Begin at the occipital ridge — the base of the skull — with gentle circular pressure
-
Work forward along the cervical lymph node chains on both sides of the neck simultaneously
-
Use gentle downward strokes along the neck toward the clavicle — following the drainage direction
-
Facial drainage: forehead toward temples, cheeks toward the jaw, jaw toward the neck
-
Ear drainage: gentle circular pressure around the ear and along the angle of the jaw
-
Eucalyptus oil (1,8-cineole) diluted in a carrier oil can be applied during massage — clinical data supports its benefit for sinonasal mucosal function
-
Three minutes is sufficient — this does not need to be a long process to be effective
For patients with significant lymphatic burden or systemic lymphatic involvement, referral to an osteopathic physician for lymphatic pump osteopathic manipulation technique (OMT) is a valuable escalation. The cervicothoracic pump and thoracic inlet techniques can mobilize lymphatic flow at a depth and efficiency that self-massage cannot replicate.
Step 3: Heat — Hot Shower or Bath
-
Heat dilates lymphatic vessels and accelerates flow through the channels
-
A hot shower is effective — a hot bath is even better, as full-body immersion provides more sustained vasodilation
-
Steam simultaneously hydrates the nasal mucosa and facilitates mucociliary clearance
-
Perform your nasal rinse immediately after the shower while the mucosa is warm, vasodilated, and primed for clearance
Step 4: Hydration — Filling the Tank
This step is not optional. It is the one that makes everything else work.
-
The lymphatic system requires adequate fluid volume to function. Lymph is approximately 95% water. When you are chronically dehydrated — as most of my patients are — the body goes into rationing mode, allocating less water to lymphatic fluid production
-
The result: even with regular movement and massage, the concentrated lymph that remains is more viscous, more difficult to move, and less effective at clearing the inflammatory and infectious burden it is carrying
-
Your daily fluid target is body weight in pounds divided by two, in ounces — adjusted upward for Arizona climate, exercise, and medication burden
-
Drink consistently throughout the day — the lymphatic system cannot process a large bolus of fluid once a day as efficiently as it can process smaller amounts distributed across the waking hours
-
Pale yellow urine is your most reliable real-time indicator that lymph fluid volume is adequate
Step 5: Sleep — Lateral Position
-
Sleep position affects both cervical lymphatic drainage and glymphatic clearance in the brain
-
Lateral sleeping — left lateral preferred — facilitates drainage of both systems compared to supine or prone positioning
-
The nasal airway restoration that we perform at SAWC — septoplasty, turbinate reduction, balloon sinuplasty — improves sleep architecture by resolving the nasal obstruction that fragments slow-wave sleep and impairs lymphatic clearance during the night
-
Most patients who have had their airway restored tell me they did not realize how poorly they had been sleeping until they experienced the difference
When the Protocol Is Not Enough
For most patients with mild to moderate lymphatic congestion — the kind that comes from a sedentary lifestyle, chronic low-grade sinus inflammation, and inadequate hydration — the daily protocol produces noticeable improvement within one to two weeks. The facial pressure eases. The drainage clears more efficiently. The morning fatigue begins to lift. The system reaches a state of homeostasis — the lymphatic tissues processing the inflammatory and infectious content they carry with enough efficiency that the immune system can stay ahead of what it is being asked to clear.
For patients with more significant lymphatic burden — those with a long history of chronic sinusitis, multiple antibiotic courses, structural nasal obstruction preventing adequate drainage, or concurrent immune dysregulation — the protocol is necessary but not sufficient. These patients need a complete diagnostic evaluation that includes nasal endoscopy, CT imaging, and a MicroGenDX nasal microbiome evaluation to understand what organism community is driving the inflammatory burden. They may need culture-directed compound antibiotic rinse therapy, surgical restoration of their sinus drainage anatomy, or in selected cases, immune support with agents like thymosin alpha-1 or LL-37.
But the protocol comes first. Always. Because no medication, no surgery, and no immune intervention will produce its full benefit in a lymphatic system that is not moving the fluid it needs to move.
Dr. G’s Clinical Pearls
-
The lymphatic system has no pump. Every structure that clears inflammation from your sinuses depends entirely on your movement, your breathing, and your hydration. A sedentary patient with chronic sinusitis is fighting the infection with one arm tied behind their back.
-
Enlarged, tender cervical lymph nodes in a chronic sinusitis patient are not a reason to panic — they are a clinical sign that the lymphatic system is working hard but has not been able to clear the burden upstream. Address the upstream problem and the nodes will follow.
-
The toe bounce at the bathroom sink costs nothing, takes two minutes, and is the most efficient lymphatic mobilization exercise available without equipment. The patients who do it consistently tell me it is the single habit that makes the biggest difference in their day-to-day congestion.
-
When lymph fluid is concentrated by chronic dehydration, movement alone is insufficient to clear it efficiently. You have to fill the tank before the pump can work properly. Hydration is not supportive care — it is a direct lymphatic intervention.
-
The head and neck self-massage is the most important video we will produce in the SAWC educational library. The technique matters — you have to follow the anatomy of the drainage pathway. Moving fluid upward, against the natural drainage direction, does nothing except waste the patient’s time.
-
When standard therapy is not working and the lymphatic burden appears significant, an osteopathic physician trained in lymphatic pump technique can produce mobilization at a depth and efficiency that self-massage cannot replicate. This is a referral I make regularly and one I would encourage every chronic sinusitis patient who has not responded to standard care to consider.
-
LL-37 is the antimicrobial peptide the sinonasal mucosa produces naturally as its first line of defense — and it is measurably deficient in patients with treatment-resistant chronic sinusitis. Thymosin alpha-1 is an immune modulator that restores the Th1/Th2 balance chronically dysregulated by long-standing sinonasal inflammation. Neither is a first-line intervention — both belong after the holistic rinse, MicroGenDX evaluation, and culture-directed compound rinse have been completed and the patient’s mucosa still has not recovered its baseline defense capacity. LL-37 is delivered as a compounded topical nasal spray applied directly to the deficient mucosal surface — approximately $80–$150 per month. Thymosin alpha-1 is a subcutaneous injection, typically 1.6mg twice weekly — approximately $200–$400 per month. You are not adding something foreign. You are replacing something the disease has taken.
-
The connection between cervical lymphatic congestion and brain fog is not metaphorical. When the lymph nodes that drain the glymphatic system’s output are overwhelmed, the brain’s ability to clear its own inflammatory waste is impaired. Treating the neck is treating the brain. These are not separate problems.
References
-
Payne SC, McKenna MK, et al. Clinical Practice Guideline: Adult Sinusitis Update. Otolaryngology–Head and Neck Surgery. 2025;173(Suppl). doi:10.1002/ohn.1344
-
Nedergaard M. Garbage truck of the brain. Science. 2013;340(6140):1529-1530. doi:10.1126/science.1240514
-
Louveau A, Smirnov I, Keyes TJ, et al. Structural and functional features of central nervous system lymphatic vessels. Nature. 2015;523(7560):337-341. doi:10.1038/nature14432
-
Aspelund A, Antila S, Proulx ST, et al. A dural lymphatic vascular system that drains brain interstitial fluid and macromolecules. J Exp Med. 2015;212(7):991-999. doi:10.1084/jem.20142290
-
Shim JY, Kim YS. The effectiveness of manual lymphatic drainage in patients with chronic sinusitis: a systematic review. Int J Environ Res Public Health. 2021;18(9):4456. doi:10.3390/ijerph18094456
-
Leduc O, Leduc A, Bourgeois P, Belgrado JP. The physical treatment of upper limb edema. Cancer. 1998;83(12 Suppl American):2835-2839.
-
Aukland K, Reed RK. Interstitial-lymphatic mechanisms in the control of extracellular fluid volume. Physiol Rev. 1993;73(1):1-78. doi:10.1152/physrev.1993.73.1.1
Want to Understand More?
This post is part of the Why Sinus Treatments Fail — And What Starts Before Them series on the Airway & Sinus Wellness Review.
→ Breaking the Biofilm: The Holistic Sinus Rinse Protocol
→ Why Antibiotics Keep Failing Your Sinus Infection
→ Does Balloon Sinuplasty Actually Work?
→ Can Sinus Infections Cause Brain Fog — or Even Look Like Dementia?
→ Browse the full Airway & Sinus Wellness Review
Why Sinus Treatments Fail — And What Starts Before Them — Patient education from the Sinus & Allergy Wellness Center of North Scottsdale.
About the Author
Franklyn R. Gergits, DO, MBA, FAOCO is an otolaryngologist and rhinologist with over 30 years of clinical experience. He is the founder of the Sinus & Allergy Wellness Center of North Scottsdale, where he performs in-office balloon sinuplasty, turbinate reduction, NEUROMARK®, and swell body reduction under local anesthesia. He performed the first balloon sinuplasty in Pennsylvania, holds dual Entellus Centers of Excellence certifications, and is the originator of the Posterior Sinonasal Syndrome (PSS) hypothesis (Preprint DOI: 10.20944/preprints202603.0858.v1). ORCID: 0009-0000-4893-6332.
SinusAndAllergyWellnessCenter.com · 480-525-8999
This content is for educational purposes only and does not constitute medical advice. If you are experiencing sinus symptoms, please consult a qualified physician for evaluation and individualized treatment recommendations.
Disclaimer:
The information provided in this article is for informational and educational purposes only and does not constitute medical advice. It is not intended to diagnose, treat, cure, or prevent any disease or medical condition. Always seek the guidance of your physician or other qualified healthcare provider with any questions you may have regarding a medical condition or treatment.
Results may vary: Treatment outcomes and health experiences may differ based on individual medical history, condition severity, and response to care.
Emergency Notice: If you are experiencing a medical emergency, call 911 or seek immediate medical attention.